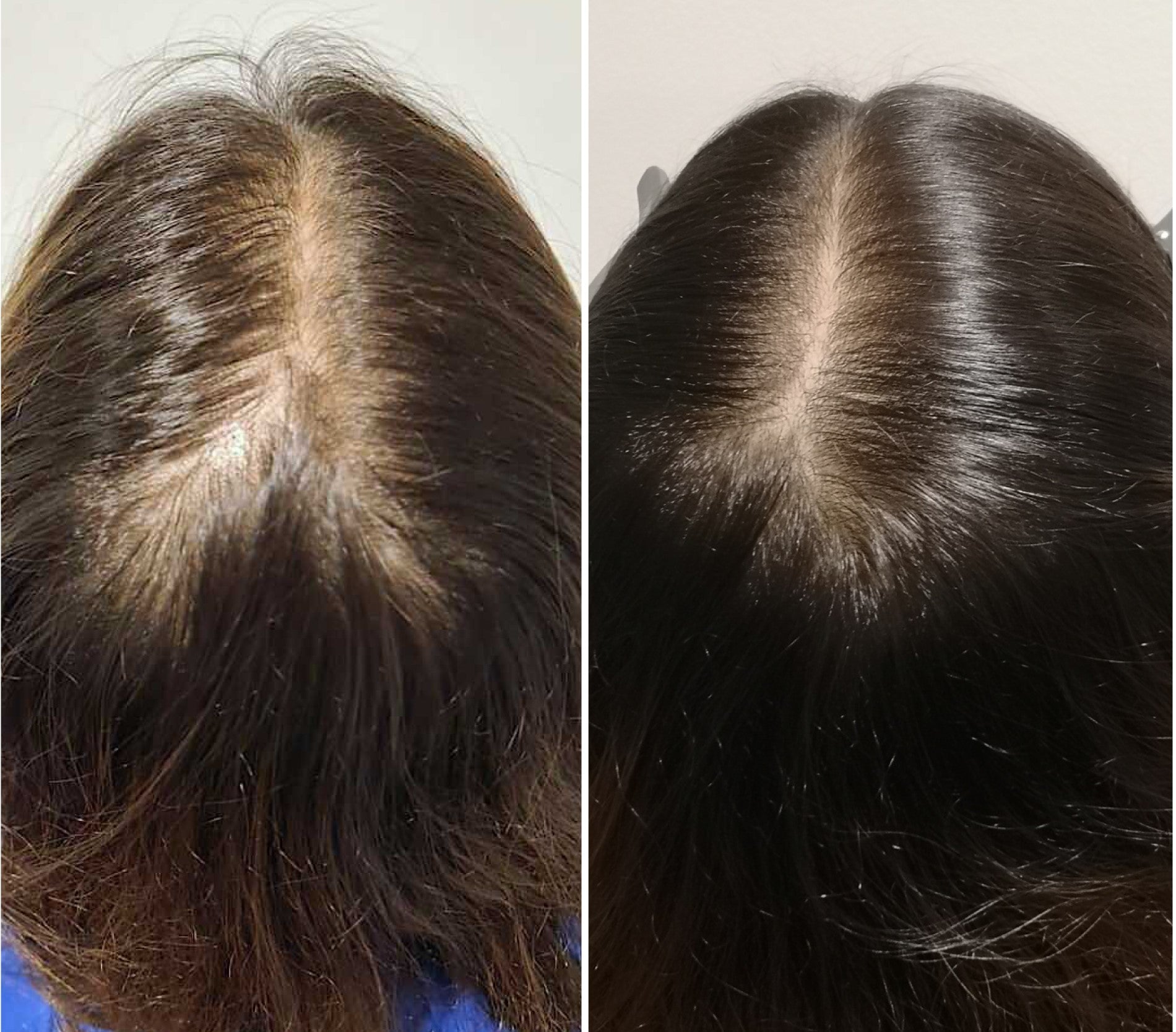
Menopausal Skin
Menopausal Skin
Skin

Menopause marks a significant transition, bringing about a cascade of hormonal changes that impact various aspects of health, including the skin. While often discussed in terms of thermal regulation or mood, the effects of menopause on the skin are profound and can alter its texture and resilience.
Understanding and Addressing Menopausal Skin Changes
This period, encompassing perimenopause and postmenopause, requires a clinical approach to skincare and aesthetic treatments to maintain skin health. Understanding these changes is the first step towards effectively managing them. Skin is highly responsive to hormonal fluctuations, particularly the decline in estrogen. Addressing these concerns involves managing specific physiological shifts occurring beneath the surface.
What Causes the Shift? The Hormonal Impact on Skin
The primary driver behind the changes seen in menopausal skin is the significant drop in estrogen levels. Estrogen is involved in maintaining skin structure, hydration, and overall function. It influences:
Collagen Production
Estrogen receptors are present on fibroblasts, the skin cells responsible for producing collagen and elastin—the proteins that provide skin with its firmness and structure. Reduced estrogen leads to decreased fibroblast activity and, consequently, reduced collagen production.
Hydration Levels
Estrogen supports the production of hyaluronic acid (HA), a natural molecule in the skin that binds to water. Lower estrogen levels contribute to reduced HA synthesis, leading to increased dryness.
Skin Barrier Function
Estrogen helps maintain the skin barrier, which protects against environmental factors and prevents excessive water loss. A decline in estrogen can affect this barrier, making the skin more vulnerable.
Sebum Production
Oil (sebum) production also tends to decrease with lower estrogen, further contributing to dryness and a change in skin luminosity.
Blood Flow
Estrogen influences blood vessel dilation and flow within the skin, contributing to nutrient delivery. Reduced estrogen can affect microcirculation.
The impact of these hormonal shifts is documented; research indicates that a significant percentage of dermal collagen can be lost within the first five years after menopause. This decline underscores why skin changes can often appear rapidly during this life stage.
Physiological Changes and Visible Characteristics
The underlying hormonal and structural changes manifest in several ways on the skin's surface. Recognising these signs is key to seeking appropriate care:
Changes in Collagen and Elasticity
The reduction in collagen and elastin leads to:
Increased Skin Laxity
Skin loses its structural support, particularly noticeable along the lower face, under the eyes, and on the neck.
Fine Lines and Wrinkles
Existing lines may deepen as the skin's structural support weakens. The texture can become more 'crepey'.
Thinner Skin
The dermal layer becomes thinner, making the skin appear less plump and more fragile.
Increased Dryness and Dehydration
Due to reduced HA and sebum production, the skin struggles to retain moisture. This manifests as:
Rough Texture
Skin feels less smooth and may appear dull.
Flakiness
Particularly common on the face and body.
Tightness and Discomfort
A persistent feeling of dryness, even after moisturising.
More Pronounced Pigmentation
Hormonal fluctuations, combined with cumulative sun exposure, can lead to changes in melanin distribution:
Sun Spots (Lentigines)
Darker spots become more apparent, especially on sun-exposed areas like the face, hands, and décolletage.
Uneven Skin Tone
General blotchiness or areas of hyperpigmentation can develop.
Melasma
While often associated with pregnancy, melasma can sometimes appear or change during perimenopause due to hormonal shifts.
Increased Sensitivity and Irritation
The change in skin barrier function makes the skin more susceptible to external factors:
Redness and Flushing
May become more frequent. Conditions like rosacea can be exacerbated.
Itchiness (Pruritus)
Dryness and barrier impairment often lead to itching.
Reactions to Products
Skin may become newly sensitive to skincare ingredients that were previously well-tolerated.
Slower Healing and Repair
Reduced cellular turnover and altered regenerative processes mean that:
Wounds Heal More Slowly
Minor blemishes or scratches take longer to resolve.
Bruising Is More Common
Thinner skin and more fragile blood vessels can lead to easier bruising.
Reduced Resilience
The skin recovers less quickly from inflammation or minor irritation.
Beyond these common signs, some individuals may also experience changes like increased facial hair or hormonal breakouts.
Clinical Approaches for Menopausal Skin Concerns
Addressing the complex changes of menopausal skin requires a multi-faceted approach. Aesthetic medicine offers solutions designed to address the specific physiological shifts occurring during perimenopause and postmenopause. At our clinic in Bondi Junction, Sydney, we utilise advanced technologies and techniques to support menopausal skin:
Restoring Volume and Structural Support (Addressing Collagen and Bone Loss)
Biostimulators
Over time, there is a natural reduction in collagen, fat, and bone density in the facial structure, contributing to skin laxity and volume loss. Biostimulatory injections work by stimulating the body's own natural collagen production over time, leading to gradual structural reinforcement. Examples include:
Sculptra (Poly-L-Lactic Acid - PLLA)
Works within the dermis to support collagen and structural integrity over several months. This is used for addressing widespread volume loss and improving skin quality.
Gouri (Liquid Polycaprolactone - PCL)
A liquid PCL injectable designed for collagen stimulation to improve skin elasticity and provide a subtle lifting effect.
Lenisna (PDLLA + HA)
Used to address volume loss and hollowing, this combines the immediate effects of Hyaluronic Acid (HA) with the long-term collagen stimulation of Poly D,L-Lactic Acid (PDLLA).
Dermal Fillers (Hyaluronic Acid)
While biostimulators focus on collagen, HA fillers are used to restore lost volume in specific areas like the cheeks, temples, under-eyes, and jawline. This provides structural support and contour, addressing the effects of fat pad changes and bone resorption.
Stimulating Collagen and Improving Texture
UltraClear™ Laser
A cold fibre laser technology offering precise epidermal ablation. It addresses pigmentation, fine lines, texture, and dullness. Recovery time varies between individuals. The Laser Coring modality of this device is used for skin tightening.
Morpheus8 (Radiofrequency Microneedling)
This treatment combines microneedling with fractional radiofrequency energy delivered into the dermis. The needles create controlled micro-injuries, while the RF energy heats the tissue, stimulating new collagen and elastin production. It is used for skin tightening, improving texture, and managing wrinkles.
Thread Lifting
Medical-grade threads are inserted under the skin to provide mechanical support to lax tissues. These threads stimulate a collagen response along their path, leading to improved skin firmness over time.
Addressing Surface Concerns: Pigmentation, Redness, and Dullness
Q-Switch Laser
Used for targeting specific pigmented lesions like sun spots by breaking down excess melanin.
AdvaTx Vascular Laser
Specifically targets redness and vascular flushing often associated with menopause or conditions like rosacea.
LED Light Therapy
Uses specific wavelengths of light to promote cellular health and support recovery from other procedures. This is a non-invasive approach for overall skin quality.
Chemical Peels
Tailored peels can exfoliate dead skin cells, improve cell turnover, and address pigmentation. The type and depth of the peel are chosen based on individual assessment.
Supporting Skin Health
Regenerative Skincare
Clinical skincare is essential. Products containing growth factors, peptides, antioxidants, retinoids (adjusted for sensitivity), and barrier-repairing ingredients (ceramides, niacinamide) are used. Specific formulations may help address hormonal effects topically. Under medical supervision, options such as topical Estriol may be discussed for collagen stimulation and skin quality.
Supplements
Supporting underlying health is important. For instance, maintaining adequate Vitamin D3 and Vitamin K2 intake is important for bone health. Supporting the facial skeleton helps maintain the underlying structure that supports the skin.
Supporting Cellular Energy with NMN
Maintaining fundamental cellular processes is a focus during aging. Nicotinamide Mononucleotide (NMN) is a researched molecule that acts as a precursor to NAD+. NAD+ is involved in cellular energy production and mitochondrial function. As levels naturally decline with age, supplementing with NMN provides the building blocks to support these essential cellular mechanisms. Always consult a medical professional before starting new supplements.
The Role of CALECIM® Professional Serum
Advanced topical treatments play a role in supporting skin health during menopause. CALECIM Professional Serum, derived from umbilical cord lining stem cells, contains a mix of growth factors, proteins, and cytokines known as PTT-6®. This technology is used for:
Supporting Collagen and Elasticity
The components in PTT-6® signal fibroblasts to support collagen and elastin production, helping to manage skin laxity and firmness.
Enhancing Hydration and Barrier Function
PTT-6® has been shown in associated studies to support the skin's own Hyaluronic Acid production, which helps manage the dryness characteristic of menopausal skin.
Promoting Skin Regeneration
By providing cellular signals, PTT-6® encourages cell turnover and skin regeneration, helping to address dullness and support the healing processes.
Managing Sensitivity and Redness
PTT-6® possesses properties that help soothe the skin and reduce redness, making it a useful adjunct post-procedure to manage recovery after treatments like lasers or Morpheus8.
Integrating CALECIM with Clinic Treatments
CALECIM Professional Serum is often integrated into a treatment plan:
Post-Procedure
Applied after treatments like Morpheus8, UltraClear, or peels to support the recovery process and manage temporary redness.
As Daily Skincare
Used regularly to support collagen production, hydration, and barrier function, complementing the results of in-clinic procedures.
For example, following a Morpheus8 or UltraClear session, CALECIM® application helps manage the skin's response and supports the regenerative processes. For patients focusing on volume restoration with Biostimulators or Fillers, using CALECIM® daily helps improve the quality and resilience of the skin.
Your Partner in Skin Health
Menopause is a natural biological process, and understanding the physiological changes allows for targeted interventions. At Beauty by Doctor, led by Medical Director Dr Phoebe Jones, we have experience in managing the specific concerns associated with hormonal changes in the skin. Located in Bondi Junction, Sydney, we offer a suite of advanced aesthetic treatments tailored to the needs of peri and post-menopausal skin.
Our approach combines technologies like biostimulators, advanced lasers, and regenerative topicals with an understanding of facial anatomy. We develop personalised treatment plans based on individual assessment.
Suitability for treatment is determined during consultation. All medical and cosmetic procedures carry risks, and outcomes vary between individuals. While complications are uncommon, it is important that potential risks, including rare adverse events, are understood. For more information, please refer to our Treatment Complications page: https://beautybydoctor.com/pages/concerns/treatment-complications